How Poor Posture Affects Your Body More Than You Think — And How to Correct It
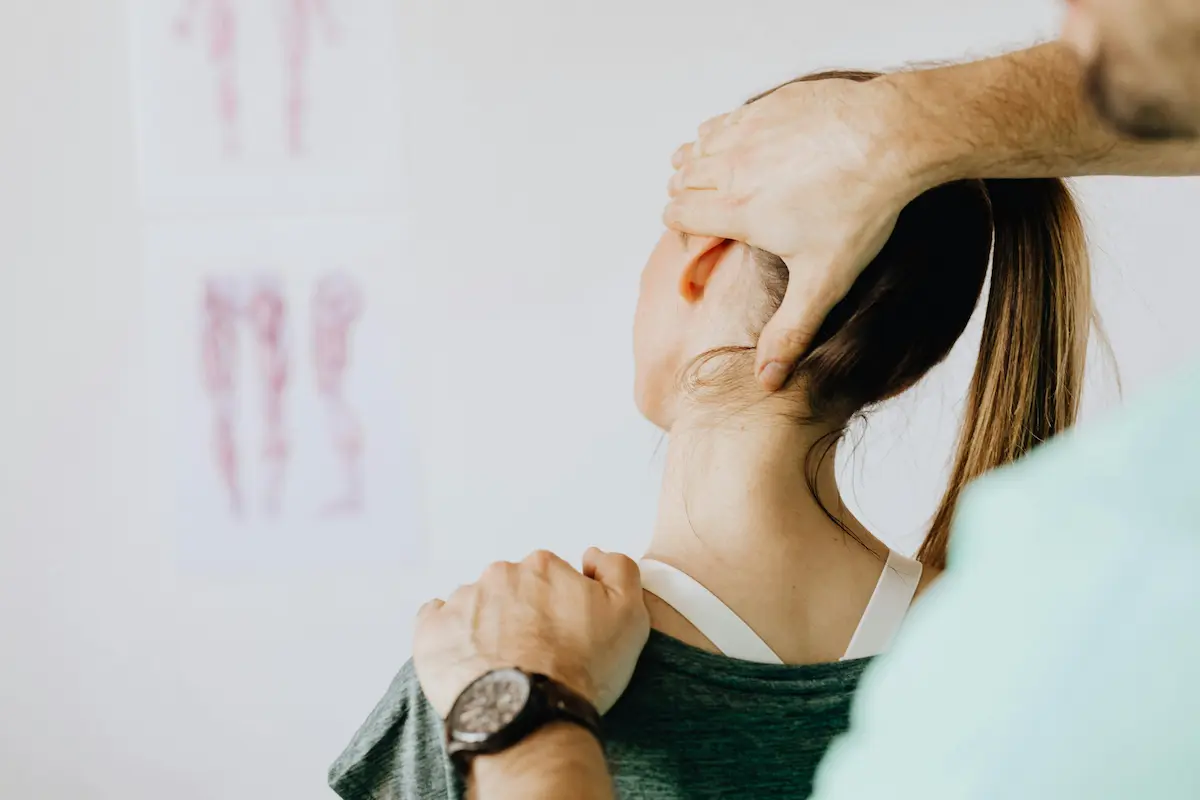
Posture is often associated with appearance, but its impact extends far beyond how someone looks. Prolonged poor posture can significantly affect musculoskeletal health, breathing efficiency, and even nervous system function.
With the increasing number of individuals working in desk-based environments, postural dysfunction has become one of the most common contributors to chronic discomfort and movement limitations.
What Happens to the Body With Poor Posture?
Poor posture places abnormal stress on muscles, joints, and connective tissues. Over time, this leads to structural and functional adaptations within the body.
Common postural patterns include:
• Forward head posture
• Rounded shoulders
• Increased thoracic kyphosis
• Anterior pelvic tilt
These changes alter how forces are distributed throughout the body, often leading to compensatory muscle overactivity and joint strain.
The Hidden Effects Beyond Pain
While pain is the most noticeable symptom, poor posture can affect several other systems.
These include:
Reduced Breathing Efficiency
Slouched posture limits rib cage expansion, reducing oxygen intake and affecting energy levels.
Altered Muscle Activation Patterns
Certain muscles become overactive (e.g., upper trapezius), while others weaken (e.g., deep neck flexors).
Increased Joint Stress
Misalignment places excessive load on joints, particularly in the cervical and lumbar spine.
Impact on Balance and Coordination
Postural instability can affect proprioception and movement control.
Why Posture Correction Is Not Just “Sitting Straight”
Many people attempt to correct posture by consciously “sitting up straight.” However, posture is not a static position — it is a dynamic function of muscle coordination and joint mobility.
Without addressing underlying issues such as muscle imbalance and restricted mobility, posture cannot be sustainably improved.
The Role of Physiotherapy in Posture Correction
Effective posture correction requires a comprehensive approach that combines assessment, movement retraining, and strengthening.
Through structured posture correction physiotherapy, clinicians can:
• Identify postural deviations and their root causes
• Improve joint mobility, particularly in the thoracic spine
• Strengthen stabilizing muscles such as the core and deep neck flexors
• Retrain movement patterns to reduce strain
At TheraTouch Physiotherapy, postural assessments are integrated with functional movement analysis to create individualized rehabilitation programs.
Evidence-Based Treatment Strategies
Modern physiotherapy incorporates several techniques:
Mobility Restoration
Improving thoracic extension and shoulder mobility reduces compensatory strain.
Strength Training
Targeting weak muscle groups restores balance and alignment.
Neuromuscular Re-education
Helps the body adopt efficient movement patterns automatically.
Ergonomic Adjustments
Small changes in workstation setup can significantly reduce postural stress.
Long-Term Postural Health
Posture improvement is not achieved overnight. It requires consistent effort and awareness.
Effective habits include:
• Regular movement breaks during prolonged sitting
• Maintaining neutral spine alignment
• Strength training for postural muscles
• Avoiding prolonged static positions
Final Thoughts
Posture is a reflection of how the body functions, not just how it appears. Addressing postural issues early can prevent long-term complications and improve overall movement efficiency.
With proper guidance and structured rehabilitation, lasting improvements are achievable.