Chronic Neck and Shoulder Pain: Why It Keeps Returning — And What Helps
Neck and shoulder pain is one of the most common complaints in modern life.
Long hours at a desk.
Poor sleep posture.
Stress that settles into the upper back.
For many people, the pain improves temporarily — then quietly returns.
Understanding why that happens is often the key to lasting relief.
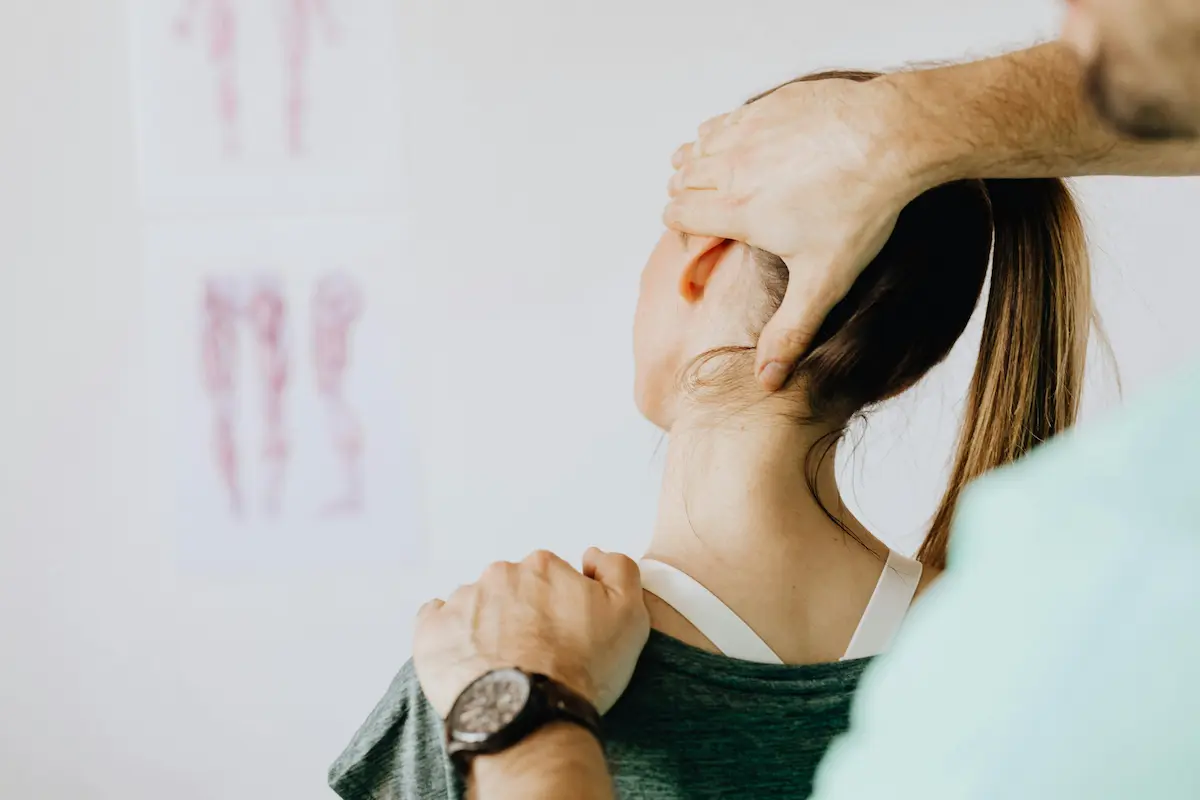
Why neck and shoulder pain keeps coming back
Pain in this area is rarely random. It often builds over time due to:
- Prolonged sitting or screen use
- Forward head posture
- Reduced upper back mobility
- Weakness in deep stabilising muscles
- Stress-related muscle tension
- Previous unresolved injuries
When certain muscles work harder than they should, they become tight and overactive. Meanwhile, supporting muscles may become underactive.
Stretching can ease the tension temporarily — but without addressing strength and control, the cycle often continues.
The role of posture (and why it’s not the whole story)
Posture does matter — but it’s not about sitting perfectly all day.
It’s more about:
- How long you stay in one position
- Whether you move regularly
- How strong your supporting muscles are
Sustainable relief usually involves improving mobility in the upper back and building endurance in the neck and shoulder stabilisers.
What physiotherapy focuses on
A structured physiotherapy assessment typically looks at:
- Cervical spine mobility
- Shoulder mechanics
- Scapular control
- Muscle activation patterns
- Workstation habits
Treatment may include:
- Manual therapy
- Targeted mobility work
- Strengthening exercises
- Movement retraining
- Load management strategies
The goal is not just to reduce pain — but to change the reason the pain keeps returning.
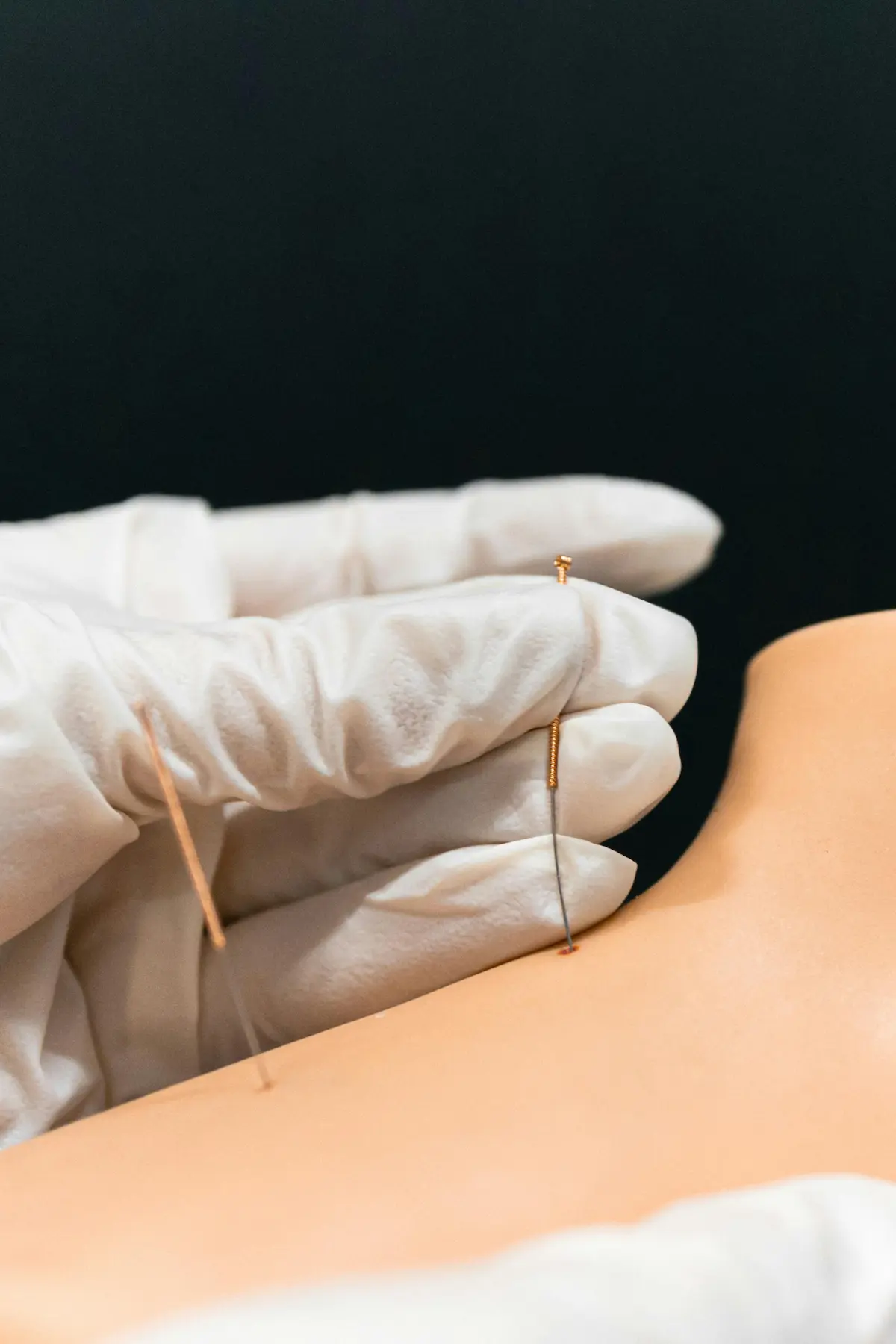
Where dry needling may help
For persistent muscle knots or trigger points, dry needling may be used as part of a broader plan.
It can help reduce abnormal muscle tension and improve movement quality — especially when combined with strengthening and posture correction strategies.
It’s typically one component of a structured rehabilitation approach rather than a standalone fix.
Signs it’s time for assessment
Consider a physiotherapy assessment if:
- Your neck pain returns every week
- You wake up with stiffness most mornings
- Headaches are linked to upper neck tension
- You feel tight even after stretching
- Pain worsens during desk work
Early intervention often prevents minor tension from becoming chronic discomfort.
Building long-term comfort and control
Chronic neck and shoulder pain often responds well to a combination of mobility, strength, and movement retraining.
With a structured plan and gradual progression, many people find that recurring tension becomes less frequent — and daily tasks feel easier.
If you’re looking for more than temporary relief, physiotherapy can help address the underlying causes and support long-term improvement.