Myofascial Trigger Points Explained — How They Cause Pain and How Dry Needling Helps
Muscle pain is often assumed to be caused by injury or strain. However, many cases of persistent discomfort originate from something less obvious — myofascial trigger points.
These small, sensitive areas within muscles can cause both localized and referred pain, making them a common yet frequently overlooked source of musculoskeletal issues.
What Are Myofascial Trigger Points?
Myofascial trigger points are tight, hyperirritable spots within muscle fibers that can:
- Cause deep, aching pain
- Limit movement
- Refer pain to other parts of the body
They are often felt as small knots or tight bands within muscles.
How Trigger Points Develop
Trigger points typically form due to:
- Muscle overuse or repetitive strain
- Poor posture and prolonged sitting
- Previous injuries
- Muscle imbalances
As a result, these factors can reduce blood flow, increase muscle tension, and contribute to the accumulation of metabolic waste, creating a cycle that maintains pain and stiffness.
Referred Pain — Why the Source Isn’t Always Obvious
One key characteristic of trigger points is referred pain, where discomfort is felt in a different area than its source.
For example:
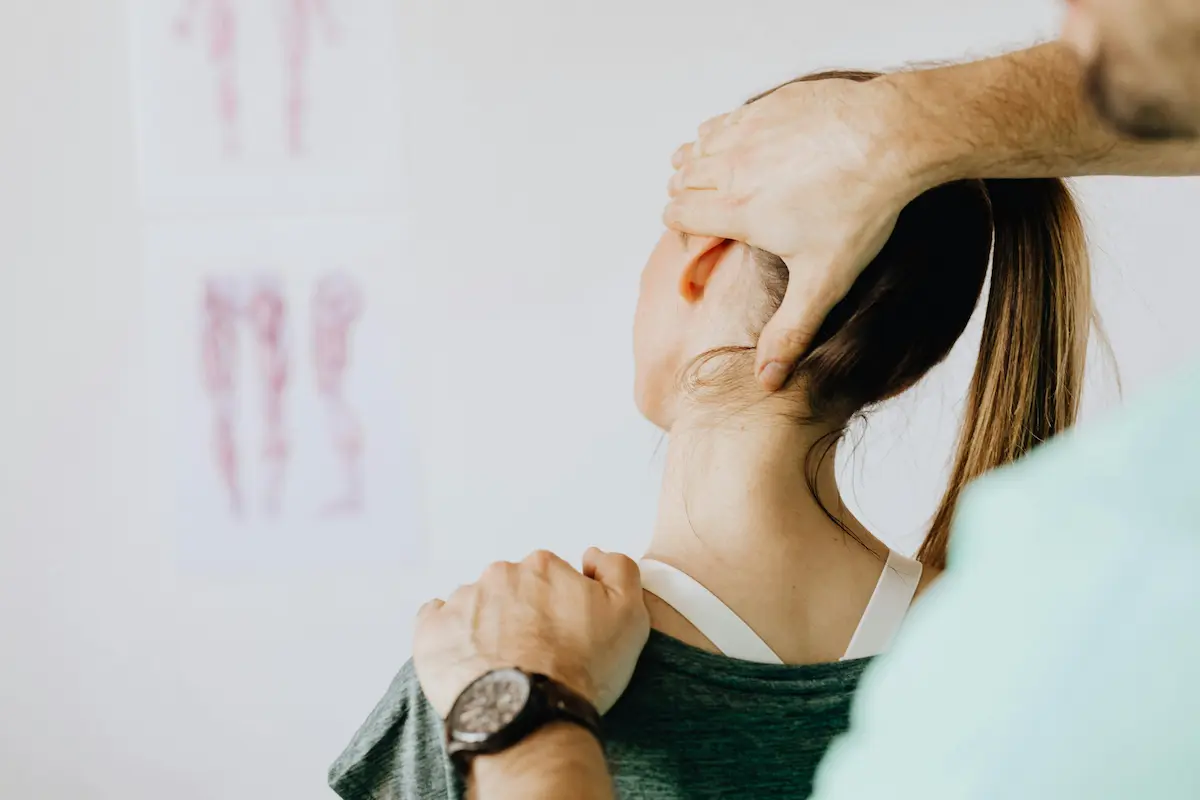
- Neck trigger points may cause headaches
- Shoulder trigger points may lead to arm pain
- Lower back trigger points may mimic nerve-related symptoms
Therefore, identifying the true source of pain often becomes difficult without a proper physiotherapy assessment.
Common Areas Affected
Physiotherapists frequently identify trigger points in:
- Neck and upper trapezius muscles
- Shoulders and rotator cuff muscles
- Lower back and gluteal muscles
- Hip flexors and thigh muscles
These regions are commonly exposed to mechanical stress and postural strain.
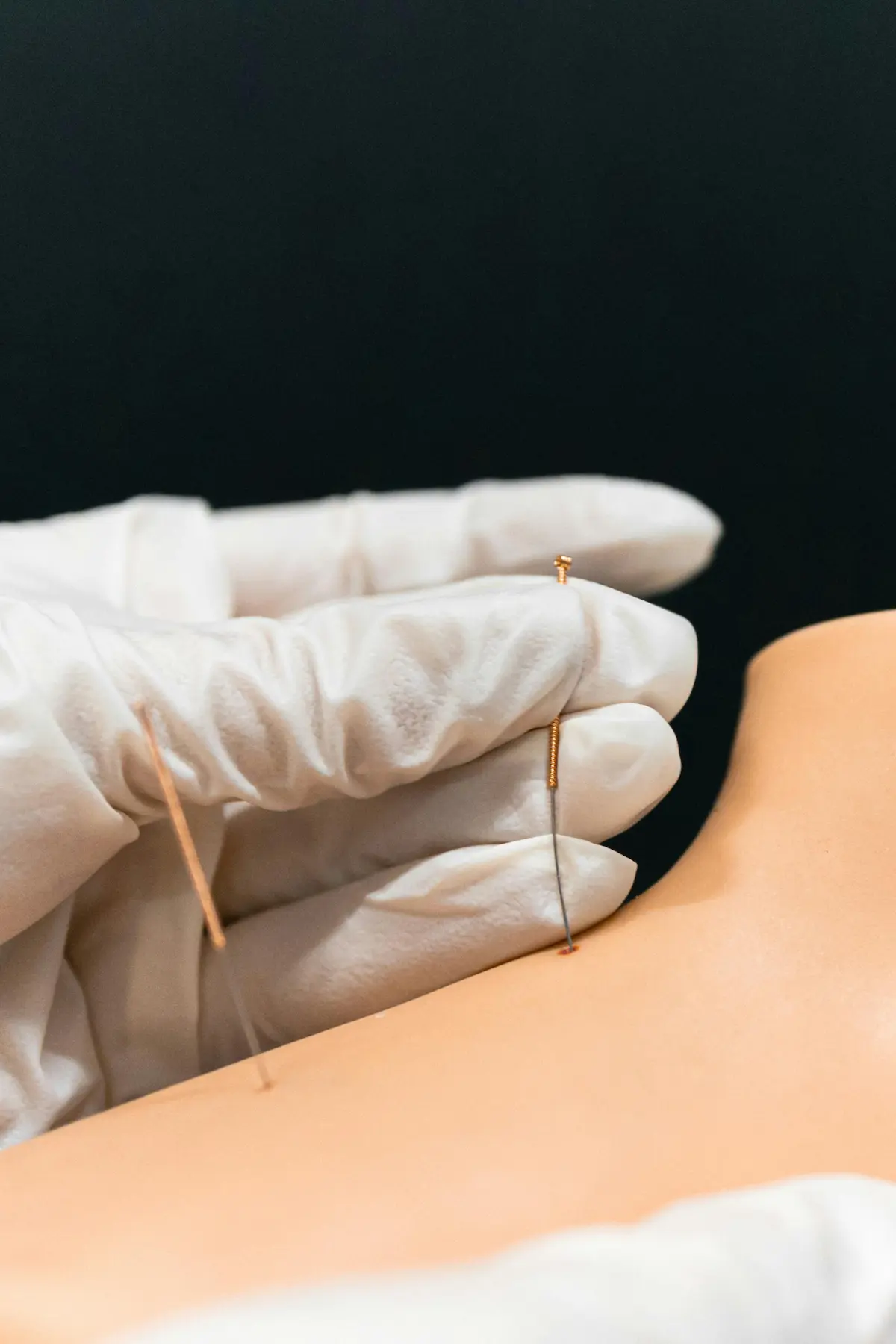
How Dry Needling Works
Dry needling is a targeted physiotherapy technique used to release trigger points.
During treatment, physiotherapists insert a fine needle into the affected muscle to:
- Reduce muscle tightness
- Improve circulation
- Decrease pain sensitivity
- Restore normal muscle function
This technique directly addresses the source of muscular dysfunction.
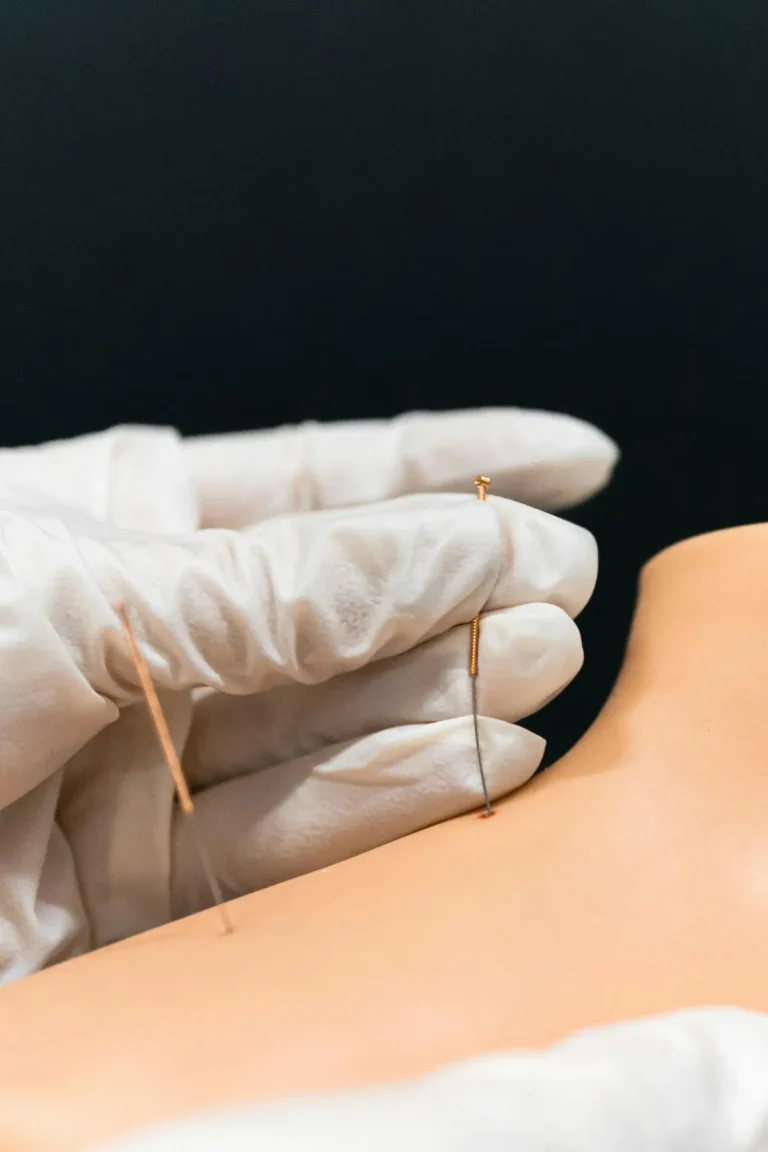
What Happens During Treatment
During a session:
- A physiotherapist identifies trigger points through physical assessment
- A thin needle is inserted into the muscle
- Patients may notice a brief muscle twitch response
This response helps release tension and reset muscle activity.
Benefits of Dry Needling
Following treatment, patients may experience:
- Reduced muscle tightness
- Improved range of motion
- Decreased referred pain
- Faster recovery from musculoskeletal conditions
Results are often noticeable within a few sessions when combined with rehabilitation exercises.
Why Dry Needling Is Combined with Physiotherapy
Additionally, dry needling is most effective when integrated into a broader physiotherapy treatment plan.
This may include:
- Strengthening weak muscles
- Improving movement patterns
- Preventing recurrence of trigger points
This combined approach supports long-term recovery rather than temporary relief.
Is Dry Needling Safe?
When performed by a qualified physiotherapist, dry needling is:
- Safe and controlled
- Minimally invasive
- Clinically guided
Some mild soreness may occur after treatment, although it usually resolves within 24–48 hours.
When Should You Consider Dry Needling?
You may benefit from dry needling if you experience:
- Persistent muscle tightness
- Pain that does not improve with rest
- Referred or unexplained pain patterns
- Limited mobility due to muscle stiffness
Early treatment can help prevent chronic conditions from developing.
Final Thoughts
Myofascial trigger points are a common source of pain that often goes unrecognized. However, addressing them requires targeted treatment combined with a comprehensive rehabilitation approach.
Through dry needling and physiotherapy, individuals can reduce muscle tension, restore movement, and support long-term recovery.
Frequently Asked Questions
What are myofascial trigger points?
Myofascial trigger points are sensitive tight spots within muscles that can cause pain, stiffness, reduced mobility, and referred pain in other parts of the body.
How does dry needling help trigger points?
Dry needling helps release tight muscle bands, improve circulation, reduce pain sensitivity, and restore normal muscle function by targeting trigger points directly.
Is dry needling painful?
Most people experience minimal discomfort during dry needling. A brief muscle twitch response or mild soreness after treatment is common and usually resolves within 24–48 hours.
How many dry needling sessions are needed?
The number of sessions depends on the severity of the condition, muscle involvement, and individual response to treatment. Some patients notice improvement after only a few sessions.
Can dry needling help chronic muscle pain?
Yes, dry needling is commonly used to help manage chronic muscle pain, tension, and movement restrictions when combined with physiotherapy and rehabilitation exercises.