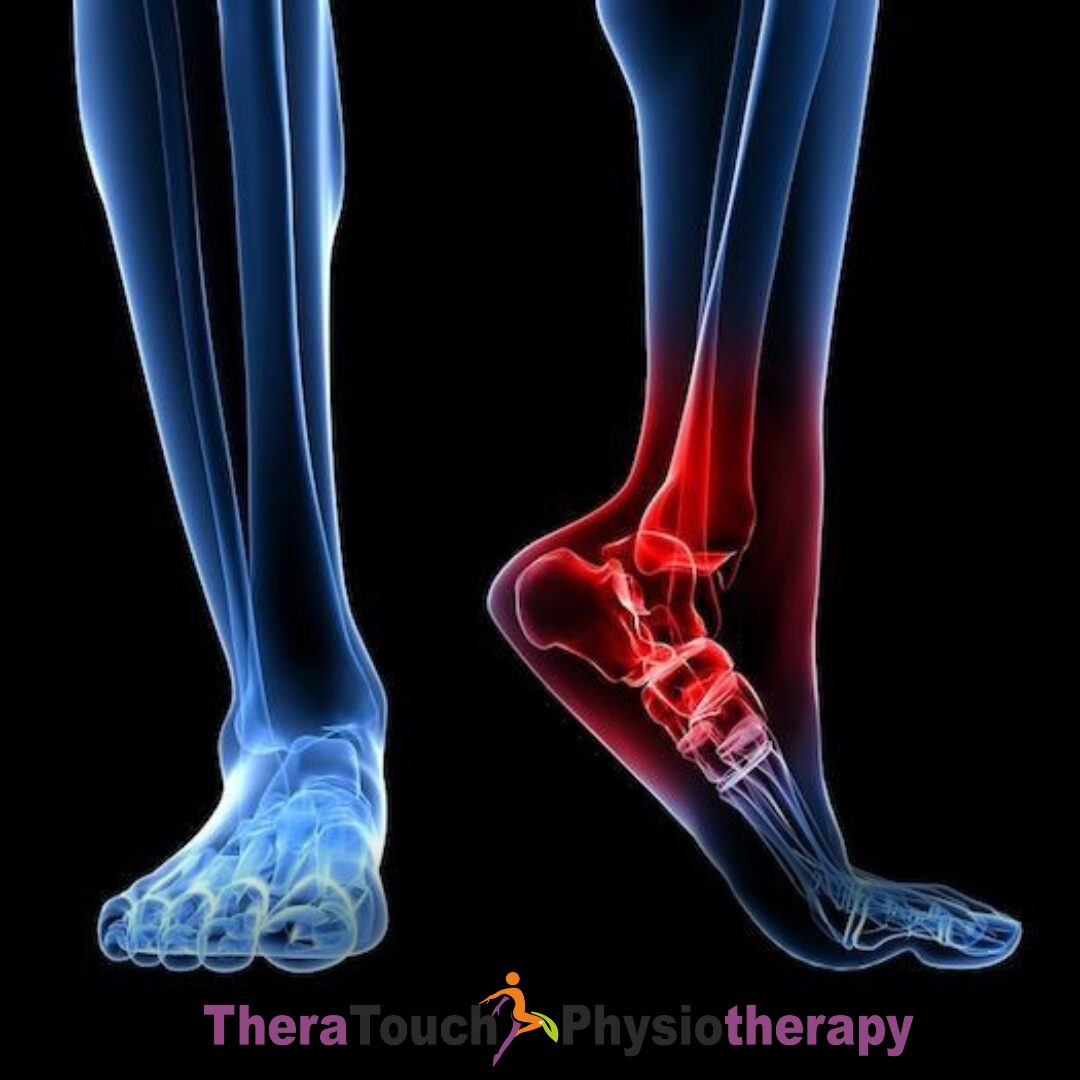
The ankle and foot form the body’s foundation during movement. Together, they support body weight, absorb impact, and allow smooth transitions during walking, running, and standing. Because these structures endure so much stress every day, injuries to the ankle and foot are both common and disruptive. Even a seemingly minor twist or misstep can result in pain, swelling, and long-term instability.
Ankle and foot injuries do not only affect athletes. People of all ages and activity levels can experience them. While some injuries heal quickly with rest, others require rehabilitation to restore strength, stability, and full function. Without proper treatment, these injuries can lead to ongoing problems with balance, mobility, and pain.
Physiotherapy provides a science-based, movement-focused approach to recovery. It does not only treat the symptoms of injury but also corrects the underlying dysfunctions that contribute to it. This article explains how common ankle and foot injuries develop, how they are diagnosed, and why physiotherapy remains one of the most effective tools for healing and long-term prevention.
Common Types of Ankle and Foot Injuries
Several types of injuries commonly affect the ankle and foot. Among the most frequent are sprains, strains, fractures, and tendon injuries. An ankle sprain occurs when the ligaments that support the ankle stretch or tear. This typically happens during a fall, a misstep, or a sudden change in direction during sports. The outer ligaments of the ankle are most often affected, leading to pain, swelling, and bruising.
Foot fractures can affect any of the foot’s 26 bones, but the metatarsals, toes, and heel bone are especially vulnerable. Stress fractures often occur from repetitive activity, particularly in runners, dancers, or workers who stand for long hours. In contrast, an acute fracture may result from a direct impact, such as dropping a heavy object on the foot.
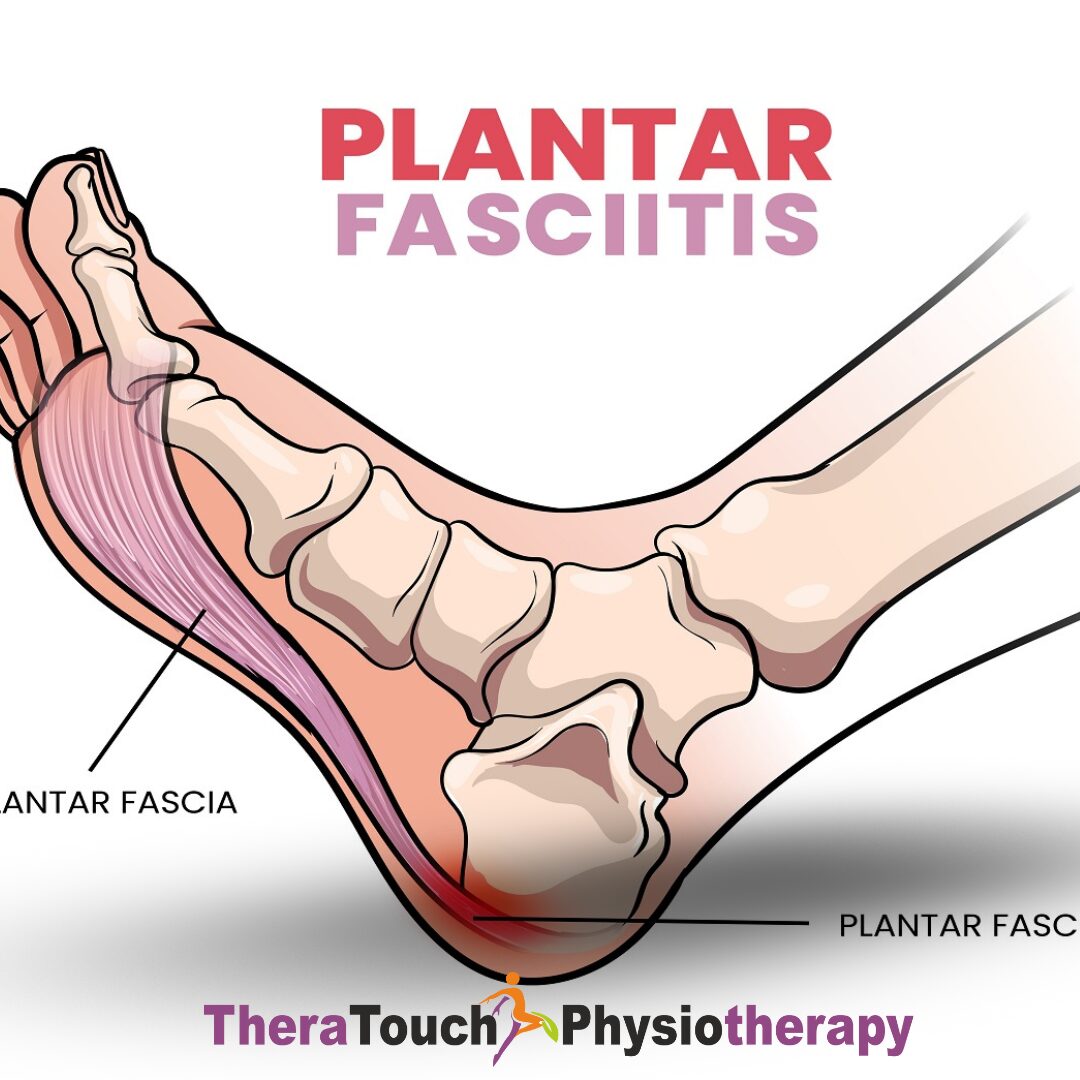
Tendinopathies are another category of injury. The Achilles tendon, which connects the calf muscles to the heel, frequently becomes irritated or inflamed due to overuse. Other tendons in the foot, such as the peroneal or posterior tibial tendons, can also become injured from repetitive strain or poor biomechanics.
Each of these injuries presents with different symptoms and requires a tailored approach to healing. What they all share is the potential to affect movement, load tolerance, and daily activity if left unaddressed.
What Causes Ankle and Foot Injuries
Ankle and foot injuries can result from a wide range of causes. Acute injuries usually involve a specific incident, such as tripping on uneven ground, landing awkwardly, or twisting the ankle during sport. These accidents may happen without warning but are more likely to occur when the body is tired, unbalanced, or poorly conditioned.
Chronic injuries build over time. Repetitive motions, poorly fitted footwear, and improper training loads contribute to gradual wear on tissues. Flat arches, high arches, or poor foot alignment can place uneven stress on bones and tendons, eventually leading to injury. Weakness in the hips, knees, or core often creates faulty movement patterns that transfer excess strain to the ankle and foot.
Poor proprioception, which refers to the body’s sense of balance and position, also plays a role. When proprioception is impaired, the risk of rolling an ankle or misplacing a step increases. This is particularly important in individuals who have already experienced a prior ankle injury, since these injuries often reduce joint stability and coordination.
Symptoms and When to Seek Help
Injuries to the ankle and foot may cause a range of symptoms depending on the type and severity. Pain is the most common indicator and can be sharp, dull, intermittent, or constant. Swelling, bruising, stiffness, and difficulty bearing weight also signal possible damage.
Some injuries, such as mild sprains or overuse conditions, may present with subtle symptoms that worsen gradually. Others, like fractures or tendon ruptures, may cause immediate, intense pain and require urgent care.
You should seek professional evaluation if pain limits movement, does not improve within a few days, or interferes with work, exercise, or sleep. Early assessment ensures accurate diagnosis and speeds up recovery. Delaying treatment often leads to compensatory issues, where other body parts are forced to pick up the slack, leading to further injury.
How Health Professionals Diagnose Ankle and Foot Injuries
Diagnosis begins with a detailed clinical assessment. A physiotherapist or healthcare provider reviews the injury history, asking how it occurred, what symptoms followed, and how it has affected function. A physical exam evaluates joint mobility, ligament integrity, muscle strength, and movement patterns.
In many cases, diagnosis does not require imaging. However, when fractures, dislocations, or serious tendon injuries are suspected, providers may request X-rays, ultrasound, or MRI scans to confirm the extent of damage. These tools are especially useful when pain remains unresolved despite conservative care. In a physiotherapy setting, clinicians take a holistic view. They do not only treat the site of pain but also examine how the injury affects the entire lower limb. Gait analysis, balance testing, and strength assessments reveal hidden weaknesses that contribute to instability or repeated injury.
Physiotherapy is Essential for Recovery
Physiotherapy plays a critical role in both short-term healing and long-term recovery. After the initial injury, swelling and pain are managed through gentle movement, manual therapy, and progressive weight-bearing activities. Early controlled movement helps prevent joint stiffness and muscle atrophy. Once inflammation subsides, the focus shifts to restoring range of motion and building strength. Targeted exercises rebuild muscle support around the injured area. Proprioceptive training, which includes balance and coordination drills, helps retrain the nervous system to stabilize the joints and prevent future sprains or falls.
In cases where the injury stems from overuse or biomechanical faults, physiotherapy addresses the root cause. Therapists correct movement patterns, improve walking and running mechanics, and prescribe home-based exercises to reinforce new habits. Education forms a central part of the process. Patients learn how to manage activity levels, choose proper footwear, and recognize warning signs before small problems escalate. Physiotherapy also prepares patients to return safely to sport, work, or active living. Rather than relying on rest or passive treatments alone, patients regain confidence through progressive, guided movement.
Long-Term Impact and Prevention
Unresolved ankle and foot injuries do more than cause lingering pain. They often lead to long-term complications, including chronic instability, early joint degeneration, and movement dysfunctions that strain other parts of the body. Even a mild sprain, if not properly treated, can reduce proprioception and set the stage for repeated injuries.
Physiotherapy reduces this risk. By building strength, coordination, and awareness, it prepares the body to handle physical demands more safely. Preventative programs that include stretching, balance work, and strength training help active individuals stay injury-free. For older adults, these programs also reduce the risk of falls and mobility loss.
Strong Steps Begin With Proper Care
Ankle and foot injuries affect how you move, work, and live. They may start with a twist, an impact, or overuse, but their effects often ripple through the whole body. Recovery requires more than rest. It calls for a plan that restores motion, builds strength, and rewires movement. Physiotherapy provides that plan. It treats not only the injury but also the person behind it. Through guided exercises, hands-on care, and education, physiotherapy helps patients regain control, reduce pain, and return to the activities that matter most. If you are dealing with an ankle or foot injury, do not wait for the problem to fix itself. The sooner you begin rehabilitation, the sooner you can take strong, pain-free steps toward recovery.